By Laura Kammerer
It’s a routine patient check until the steady cadence of beeping monitors turns to
a long tone.
As a USC nursing student rushes to the patient, searching for clues about why he is deteriorating, the phone rings. Another patient’s lab results are ready. While listening to the patient’s chest with a stethoscope, another interruption. A family member is requesting an update.
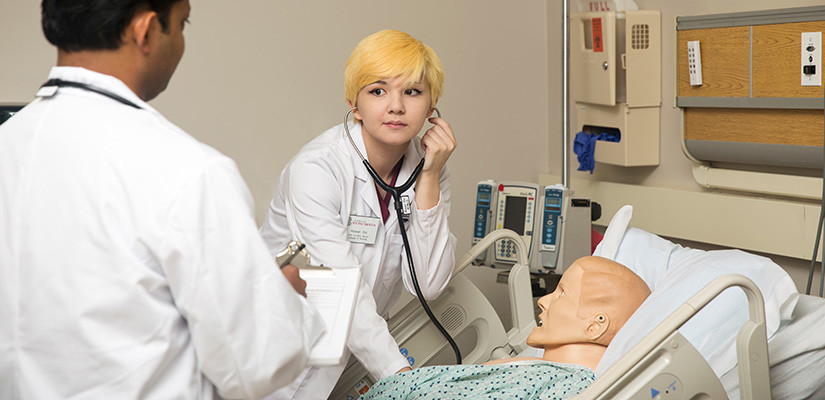
It’s the real world of nursing where caregivers act as cognitive detectives while juggling competing demands. At USC, nursing students first encounter these scenarios at the College of Nursing’s 5,300-square-foot simulation lab, which opened in 2009.
“The power and magic of simulation is the ability to help students be able to pull the pieces together from their different areas of learning and apply it in a setting that’s controlled,” lab director Rachel Onello said. “It allows them to enter the zone of proximal development where they can make mistakes and they can try out new thinking skills and work at the edge of their expertise without harming patients.”
Once a novelty centered on student practice with task-oriented care skills such as injections or wound care on mannequin arms or legs, simulation learning has gained traction in nursing education as research began to demonstrate its benefits for student learners, including the landmark 2010 study by the National Council School Board of Nursing that studied simulation at USC and nine other schools of nursing.
At Carolina, simulation continues to take center stage. The College of Nursing in January hired renowned simulation expert Onello as its director and in July promoted clinical assistant professor Crystal Graham to a newly created assistant director position, both of whom are certified in clinical simulation education by the Society for Simulation in Healthcare.
Building on the college’s simulation education strengths — the learning modality has been integrated throughout clinical courses in both the undergraduate and graduate nursing programs, with nearly 6,300 hours of student simulation learning logged this year from January through late August — Onello has set a bold course for the lab: to be the one of the first SSH-accredited simulation labs accredited in a college of nursing in the southeast.
The college has many of the key components in place: supportive leadership, faculty buy-in, a quality facility and a dedicated simulation team consisting of Onello, Graham and operations manager Lonnie Rosier as well as a newly formed simulation advisory committee. Still, Onello anticipates that it will take about two years to prepare and submit the college’s application.
“Being accredited is an external mark of excellence that an external group of experts has looked at your program thoroughly and said, ‘Yes, you are doing things according to standards of best practice and doing it in a very thoughtful and intentional manner that really contributes to improved outcomes for your learners,’” she said.
“Ultimately that is what we’re all about here at the College of Nursing, striving for excellence and striving to be a leader not only in best practices but in innovation.”
Rachel Onello, Lab Director
Inside the magic
To an outside observer, the simulation lab appears to be a sophisticated practice field: a place where students execute steps and procedures they’ve learned in class.
But the simulation itself provides only a fraction of the learning experience.
First, students gather with a faculty member for a pre-briefing where they receive information about the scenario they’re about to enter, including background patient data and assumptions.
Next, in small groups, students enter their assigned simulation exam room, either one of two dedicated maternity patient simulator rooms or six flexible rooms that can be staged as medical-surgical patient simulator rooms, psychiatric or standardized patient exam rooms. Each room is equipped with sophisticated pre-programmed mannequins that include features such as chest rising, blinking eyes, heart and lung sounds, blood pressure and pulse.
In some instances, trained human patients are employed instead of the high-tech mannequins. Historically the college has utilized these standardized patients for training students in psychiatric care, but starting this fall students will practice assessment, patient communication and problem-focused exams with standardized patients, with nurse practitioner students utilizing them this spring to conduct breast, gynecological, rectal and prostate exams, Onello said.
During the clinical scenario, some students actively participate while their peers observe, taking detailed notes about their classmates’ decisions and actions. A faculty member runs the pre-programmed exercise from a control room and records the session.
The goal is to challenge but not overwhelm students with realistic scenarios that directly tie to course learning objectives and outcomes, Onello said. Students are coached that “gotcha” moments are not part of the simulation experience, which is never designed to trick or confuse learners. If students open a cabinet to administer medication and it’s missing, they are forced to think about what they would do in the hospital setting, she said. How would they resolve the situation? What resources are available? Who would they call?
Once the scenario has finished (typically no longer than 20 minutes), the faculty member and students gather for the debriefing where decisions are dissected and analyzed by every team member. Faculty members can reinforce good decisions and thinking patterns, clarify knowledge gaps and refine trouble spots to help students avoid getting stuck, Onello said.
Debriefing at Carolina is successful in part because of the college’s philosophy that students are intelligent and capable and enter the lab aiming to do their best. To empower students to become better nurses, during debriefing “their mistakes are not (treated as) crimes to be punished but rather puzzles to be solved,” Onello said.
This fall, the college has introduced a new evidence-based approach to debriefing that stimulates deeper discussions and analysis of student decision-making, said Onello, who authored three chapters in the National League of Nursing’s forthcoming guide to faculty training.
After debriefing, the students may swap roles, becoming caregivers rather than observers and vice versa, and then re-enter the simulation suite to conduct another scenario. Simulation experiences typically last either four or eight hours total.
Spreading simulation’s impact
Onello envisions Carolina’s nursing simulation lab becoming a hub where best practices can be shared with other teams to elevate simulation education across the region and state for student learners and practicing nurses alike. To that end, she is helping to support the launch of the Midlands chapter of the Carolinas Healthcare Simulation Alliance by hosting the fall meeting for simulation educators across North and South Carolina and identifying opportunities to work with clinical practice partners as well as the USC system campuses in Lancaster, Salkehatchie and Aiken.
“We are preparing more safe and competent health care professionals through simulation,” Graham said. “We’re not only benefitting students. We’re improving the lives of those in our communities.”