Living in a rural community brings lots of advantages: close-knit communities, easy access to nature, less noise and pollution, lower home prices. But a lack of population density also brings challenges, and access to health care is one of them.
In South Carolina, six in 10 adults suffer from a chronic disease such as heart disease, stroke, cancer or diabetes, according to the S.C. Department of Health and Environmental Control. Four in 10 suffer from more than one. These challenges hit especially hard in the state’s small towns and sparsely populated areas, where there are fewer doctors, nurses and hospitals than in Columbia, Charleston or Greenville.
As daunting as the state’s health issues can seem, the University of South Carolina is well positioned to help.
- Clinical faculty at the university have embraced telehealth as a way to increase access to health care services in underserved areas of the state.
- The university is developing a Brain Health Network to improve diagnosis and treatment of Alzheimer’s disease and other dementias.
- Systemwide, the university awards 900 nursing degrees per year, helping to meet a pressing need for new nurses.
- Both the School of Medicine Columbia and the School of Medicine Greenville rank in the top 10 nationally for their number of graduates working in medically underserved communities.
Here are some of the ways in which university researchers and alumni are working to advance the health of South Carolina residents.
When Elizabeth Crouch finished her doctorate in policy studies, she didn’t even realize there was a research field devoted to rural health.
Now, 10 years later, the health services policy and management associate professor in the Arnold School of Public Health has been recognized by the National Rural Health Association with its 2023 Outstanding Researcher Award.
Crouch, who also directs USC’s Rural and Minority Health Research Center, was honored for her work examining health disparities among rural and other vulnerable populations — from adverse childhood experiences to Medicare utilization in older adults. She is particularly interested in the positive and adverse experiences faced by the more than 10 million children living in rural America.
“The rural kids have higher rates of poverty, which is an adverse experience because there are also other stresses that come along with that,” Crouch says. “But we also know there are a lot of social networks and positive and social supports in rural communities as well. It’s being able to tell that full story of what people are experiencing and what kids are experiencing. It gets into the social determinants of health – what do kids and families need in rural America? That’s my big passion.”
Learn more about Elizabeth Crouch
Imagine your child is diagnosed with a heart condition. You need to take unpaid time off to get her to doctor’s appointments, and you don’t have reliable transportation to get to specialists in Columbia, Greenville or Charleston – a few hours from your home.
Enter the South Carolina Center for Rural and Primary Healthcare at the USC School of Medicine Columbia.
The center works to improve health care delivery for rural communities by operating and facilitating a range of programs. Through one, the Department of Pediatrics sends subspecialists – doctors who specialize in over 18 conditions such as children’s asthma, heart ailments or diabetes – into areas outside the state’s urban hubs.
The subspecialists go to smaller communities and set up clinics in a leased space or at a primary care doctor’s office. The service helps the patients, who can be seen by a specialist nearby instead of making a long trip. And it improves the odds that they will make their appointments. In the past, specialists often had no-show rates of 50 percent or higher from out-of-town patients. When children see specialists on a regular basis they are able to better manage their conditions and avoid the emergency room.
“Rural health care is so different because of distances and access to providers,” says Kevin Bennett, the center’s director. “For example, there is no way a place like Lancaster could or should support a pediatric cardiologist, right? But those kids deserve that care in person as well.”
Serving children in rural areas
New nurse Makenzie Edwards could tell the woman was feeling lonely. The patient had been brought to Union Medical Center for monitoring, but once her stay was over, she would be going back to her nursing home. So Edwards did what nurses do best – she went above and beyond to make her patient feel special.
Her efforts lifted the woman’s spirits, and Edwards found herself uplifted, too.
“She told me that I was going to be a really good nurse,” Edwards says. “It reminded me that this is what I want to do. This is why I want to do it. I want to make a difference in people’s lives, and I want to be there for them when they’re vulnerable.”
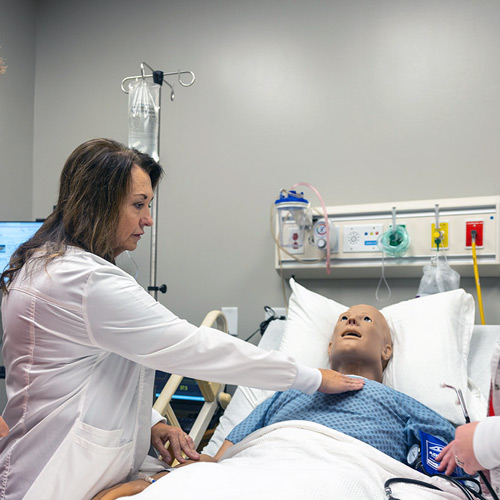
Edwards is one of six nurses to graduate from the first-ever bachelor’s in nursing cohort at USC Union through a partnership with USC Aiken. The partnership, which also includes a program at USC Sumter, is designed to address the nursing shortage in South Carolina, particularly in areas like Union, a city of just 8,000 people.
The USC system has been on a mission to increase the number of registered nurses statewide. BSN degrees are offered at the Columbia campus and each of the comprehensive universities: USC Aiken, Beaufort and Upstate. Degrees are also offered in conjunction with a four-year institution at USC Lancaster, Salkehatchie, Sumter and Union. A few campuses offer online BSN programs for students who already have a two-year or three-year nursing degree. All told, the USC system awards 900 nursing degrees each year.
For Edwards, who grew up in Union and has a strong support system there, the prospect of attending nursing school without leaving home was an easy sell. She isn’t alone.
“These students don’t want to leave home,” says Katie Chargualaf, interim dean of USC Aiken’s School of Nursing. “They want to help their local communities. So, we’re going to keep that ball rolling and we’re going to meet the needs in these communities.”
When Patti Fabel began as executive director of the Kennedy Pharmacy Innovation Center, she wanted to find a way to show stakeholders the value of having more pharmacists in rural, underserved areas.
“Here in the College of Pharmacy and in the profession, we already know that pharmacists can have an impact on patient care, particularly when collaborating with physicians,” says Fabel, a clinical associate pharmacy professor. “But it’s the business model piece and the sustainability that is needed which makes it difficult for that to happen.”
In 2018, a five-year grant was secured for a demonstration project to promote and expand team-based care with a training program that would integrate pharmacists into primary care practices.
“The hypothesis was that if we can give them just a little bit of funding and a little taste of what a pharmacist could do for them in these small pilots that they’d want more and they would try to figure out a way, through our help, to make it sustainable and keep the pharmacist.”
The idea is working. Partnering with federally qualified health centers, independent pharmacies and family care providers, Fabel and her team are showing how patients can benefit when pharmacists and doctors work together as a team to manage care. If cost is an issue, for example, a pharmacist can offer an alternative.
“I think doctors need the pharmacist perspective,” says John Pugh, who earned his Pharm. D. in 2005 and is now president of Prosperity Drug Co. “And we oftentimes need the medical perspective.”
A team approach to treatment is helpful for the patient, too, to gain a more holistic view of their condition and what they can do about it.
“It’s their health, right?” Pugh says. “It’s our job to make sure they’re educated. They can’t make a good decision without the appropriate inputs.
Fabel notes that the end of their trial has coincided with an increase in federally qualified health centers across South Carolina that have incorporated clinical pharmacists into what they do.
“To actually see the pharmacist there during the day helping you with patients, it changes perceptions," she says. “And it was great to see their buy-in and excitement with having a pharmacist and willingness to try something different.”
Being a new or expectant mother can be dangerous, even deadly. In 2021, more than 1,200 women in the United States died during pregnancy or in the six weeks following delivery. And Black women are three times more likely to die from a pregnancy-related cause than white women, according to the Centers for Disease Control.
Mothers and children are especially vulnerable in South Carolina, where inadequate prenatal care and high rates of conditions such as hypertension and diabetes can cause pregnancy complications.
But it doesn’t have to be that way. According to the CDC, five in six pregnancy-related deaths are preventable; meanwhile, other maternal health risks can be greatly reduced through proper intervention.
Across campus, USC’s researchers are on a mission to assist in that effort.
A collaborative approach: Robin Dail is the director of the Perinatal, Pediatrics, and Family Research Center, an interdisciplinary center dedicated to improving maternal health outcomes. “Much of our research is aimed at preventing neurologic developmental delays and other health challenges in children born premature,” says Dail, health sciences endowed professor at the College of Nursing. “We know families experience socioeconomic stress due to complications from prematurity. We aim to decrease that burden on families and, ultimately, society.”
Mapping birth inequities: As part of a student project last year, Honors College senior Taylor Olson developed a comprehensive map of perinatal services in South Carolina. It was an eye-opener for many. “When you look at birth equity, rural areas are more predominantly African American and Hispanic,” says Kathryn Luchok, a senior instructor in the Department of Women’s and Gender Studies who supervises student projects on birth equity at the South Carolina Birth Outcomes Initiative. “So if you don’t address the needs there, you’re also not addressing the needs for people of color who have less than stellar outcomes in the state to begin with.”
Dedicated to lasting change: Peiyin Hung, deputy director of the Rural and Minority Health Research Center at the Arnold School of Public Health, studies rural health disparities and their impact on maternity care. But she’s not just studying the issues – she’s also working to solve them through policy change. In fact, her dissertation helped inform the federal Improving Access to Maternity Care Act. “This is my passion – to solve health disparity issues and inform policymakers and decision makers for necessary actions,” she says.
More than a quarter of South Carolinians live in rural areas, which brings them a set of unique challenges that their urban counterparts don’t face. Many remote communities are medically underserved and lack access to public transportation.
Enter Jessica Seel, who earned her master’s degree from the Arnold School of Public Health in 2016. She serves as director of behavioral health initiatives and workforce development at the South Carolina Office of Rural Health.
Seel, from West Columbia, discovered her love of rural health while interacting with people from small towns throughout the state as she worked her way through the ranks of a health care company.
“Seeing disparities in action and seeing them in my own life, I developed this huge passion to advocate for change, to advocate for equality, to advocate for individuals who weren’t born into a situation that afforded them the opportunities that others may have,” she says. “Remembering those times and those feelings drove me to this work.”
Seel, who works with advocates, stakeholders and others, says it’s important to let communities lead the way in identifying their own needs. She’s met champions in communities across the state who are addressing health issues such as opioid use disorder, suicidal ideation, HIV and mental illness. Seel’s job is to bring everyone to the table and connect them with the resources they need to move forward.
“I love breaking down barriers, letting different sectors work together, whether it is community members, individuals with lived experience, policymakers or health care professionals,” she says. “It’s about taking away those titles and having them just work as community members collaboratively. That’s where real change happens.”
Fifteen years ago, Julie Smithwick was a community health worker focused solely on new Latino mothers and families in South Carolina.
Today, she directs a new center in the Arnold School of Public Health that’s training hundreds of community health workers who assist vulnerable populations with health and social needs ranging from children with disabilities to adults with chronic diseases and more.
Smithwick’s successful track record has earned trust from government agencies, including the S.C. Department of Health and Human Services, which recently awarded the Center for Community Heath Alignment $3.6 million to train and equip community health workers and organizations around the state to help people without insurance address health and social challenges.
“Our priority populations are communities that experience the highest health inequities in South Carolina and beyond,” Smithwick says. “There is a lot of evidence that the community health worker model is effective – that trusted members of a community are sometimes the most effective people to connect their peers and neighbors to food or housing or mental health and medical resources.”
Now, through the university’s Center for Community Health Alignment which she directs, Smithwick is overseeing a pilot program called Community Health Workers Changing Outcomes in South Carolina. The program works with 14 community-based organizations and federally qualified health centers throughout the state. Among those organizations are Care South, a federally qualified health center in the state’s Pee Dee region; the Bee Initiative, a community-based doula program in the Lowcountry; and Family Connection, a statewide community-focused organization that supports parents of children with disabilities.
“We’ve got a presence and a footprint all over the state, and we’re really trying to help build the capacity of the community health worker workforce that can address some of our state’s most pressing needs,” she says.
EMPOWERING COMMUNITY HEALTH WORKERS