August 25, 2020 | Erin Bluvas, bluvase@sc.edu
Scientists from across the Arnold School, including the Department of Health Promotion, Education, and Behavior (HPEB) and the Department of Epidemiology and Biostatistics, have collaborated to develop the first comprehensive obesogenic environment (i.e., an environment that promotes weight gain/deters weight loss) index for youth in the United States. Published in the International Journal of Behavioral Nutrition and Physical Activity, this study was led by HPEB associate professor Andrew Kaczynski and epidemiology and biostatistics associate professor Jan Eberth through the Rural and Minority Health Research Center. The researchers found a higher prevalence of obesogenic counties in rural areas and in the South.
“Childhood obesity has become a major threat to public health in the United States, where one third of children and adolescents are overweight or obese – more than three times the rate of 30 years ago,” Kaczynski says.
Obese children are more likely to become obese adults and have an increased risk for high blood pressure/cholesterol, type 2 diabetes, asthma, sleep apnea, and fatty liver disease. They also have an increased risk of death from hypertension, stroke, and some cancers.
While the causes of excess weight gain are complex, most researchers agree that obesity occurs when more calories are consumed than expended (i.e., energy imbalance). Previous studies have already shown that environment plays a key role in unhealthy diets and physical inactivity.
For example, do residents in a community have access to affordable fresh fruits and vegetables? Safe walking paths? Playgrounds?
“Diverse environmental factors are associated with physical activity and healthy eating among youth,” says Kaczynski, who researches how these factors impact health in his Built Environment and Community Health (BEACH) Laboratory. “However, no previous study has created a comprehensive obesogenic environment index that can be applied at a large geographic scale.”
To create such an index, the authors reviewed 20 review articles and gathered input from 12 experts to identify community-level variables associated with physical activity, healthy eating, or overweight/obesity among youth for potential inclusion the index. The final 10 variables included the number per 1,000 residents of grocery/superstores, farmers markets, fast food restaurants, full-service restaurants, and convenience stores, as well as the percentage of births at baby (breastfeeding)-friendly facilities. They also examined the percentage of the population living close to exercise opportunities, percentage of the population < 1 mile from a school, a composite walkability index, and the number of violent crimes per 1000 residents.
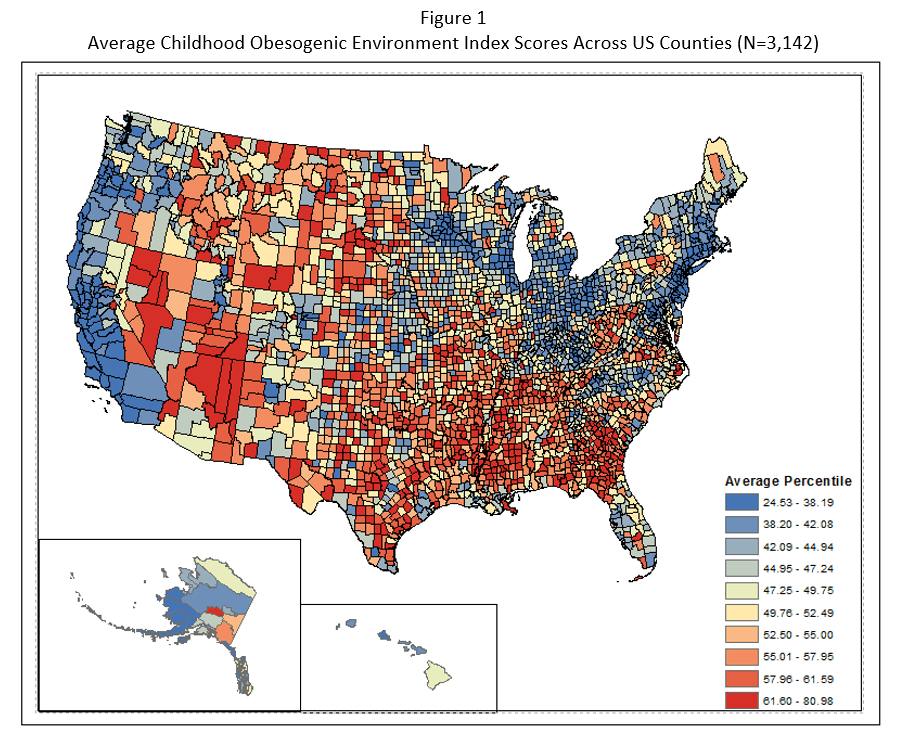
The research team compiled publicly available data related to each variable for every county in the United States. They found that obesogenic counties were more prevalent in the South, compared to the Northwest, Midwest, and West regions. They also found a higher prevalence among rural counties when compared to metropolitan counties – across the country (see map above).
“These findings suggest that public health interventions in the South, particularly in non-metropolitan counties, should incorporate environmental supports for healthy behaviors and address residential segregation that creates greater access disparities,” says Eberth, who directs the Rural and Minority Health Research Center and is the Geospatial Core Lead for the UofSC Big Data Health Science Center. “More broadly, the comprehensive childhood obesogenic environment index we created can be applied to benchmark obesogenic environments and identify geographic disparities and intervention targets as well as examine associations with obesity and other health outcomes.”
The authors note that physical environments could be modified to promote physical activity and increase access to exercise opportunities, such as improving walkability and pedestrian/bicycle safety through infrastructure improvements (e.g., sidewalks, traffic calming measures). Partnering with rural schools to adopt programming (e.g., Safe Routes to School) and establishing physical activity-related policies (e.g., shared use agreements to increase accessibility of school recreation facilities/playgrounds to the public) offer additional opportunities to increase exercise in rural communities.
Environmental features can also be modified to increase the availability of healthy food options. For example, policy makers could use food outlet zoning to reduce the prevalence of food swamps (i.e., unhealthy food outlets such as fast food restaurants and convenience stores) around schools. Rural public health agencies could also partner with schools, grocery stores, and restaurants to bring healthier food options into schools and restaurants and sponsor farmers markets.
“These efforts to increase access to healthy food options could contribute to reducing the number of food deserts in rural areas,” Eberth says. “Through a number of different public health policies and initiatives, we can work to overcome barriers to healthy living.”
This study was supported by the Federal Office of Rural Health Policy (FORHP), Health Resources and Services Administration (HRSA), U.S. Department of Health and Human Services (HHS) under cooperative agreement # U1CRH30539. The information, conclusions, and opinions expressed in this brief are those of the authors and no endorsement by FORHP, HRSA, or HHS is intended or should be inferred.
Related:
Jan Eberth named 2020 Outstanding Researcher of the Year by National Rural Health Association
HPEB’s Andrew Kaczynski awarded NIH grant to advance mobile app for collecting data to improve parks